Stick To Your Colitis Treatment Plan To Avoid Overusing Steroids
Some people may worry about side effects that can be caused by their maintenance medication and they ditch their treatment while theyre in remission. According to a PLoS One, nearly half of inflammatory bowel disease patients stop taking their medication for a variety of reasons. But doing so increases the risk of relapse.
Although steroids can have dangerous side effects, you should take them as directed if you need them. The same goes for your maintenance medication.
The most important thing to know with UC is that how you feel doesnt correlate with whats happening on the inside, Hudesman says. Even if you feel great most of the time without medication, if I did a colonoscopy, it might show severe disease. A lot of patients tolerate little flares until they cant. Then all of a sudden, youre talking about surgery or a very complicated disease.
RELATED: Thinking of Stopping Your Ulcerative Colitis Medication? Think Again
The bottom line? Every patient is different. But if youre experiencing severe UC flares, you may need a steroid initially until your maintenance medication can control your condition. The various side effects associated with prolonged steroid use give many doctors pause.
Steroids are fast and cheap and well-known, but we prefer to get a flare under control without them if we can, Raffals says.
You may also need to experiment with maintenance medication until you find one that works, or switch to immunosuppressant or biologic therapy.
Can Intermittent Fasting Help Autoimmune Diseases
Intermittent fasting reduces inflammation, corrects insulin resistance, gives the gut a rest, helps repair the leaky gut*,and repairs your cells* all which help heal autoimmune diseases. I urge you to spend some time reviewing peoples testimonials and how fasting aided their healing journey. If you suffer with an autoimmune disease its worth looking into the awesome benefits of fasting.
If your looking to improve your IBD and change your life, check out my free healing guide.
What Is A Good Breakfast For Colitis
A few stomach-friendly breakfast ideas:
- 1 cup of low-fat cottage cheese with a fruit cup.
- 2 scrambled eggs with ½ cup of unsweetened applesauce.
- 1 cup of oatmeal with a peeled peach.
- Smoothie made with 1 cup of low-fat Greek yogurt, 1 cup of unsweetened almond milk, 1 cup of frozen peaches, and ½ banana.
You May Like: What Foods To Eat When Fasting
Crohns Disease And Ulcerative Colitis And Digesting Food
Your mouth and stomach break down food by mechanical and chemical means. When the food has reached a pulp-like consistency, it is slowly released into the first part of the small intestine . The food is then massaged along the length of the small intestine. Organs like the pancreas and the gall bladder make digestive enzymes to further break down the food into its simpler components.
The small intestine is lined with microscopic , finger-like projections that lie close to tiny blood vessels . Nutrients pass into the bloodstream through these villi. The rest of the food is pushed into the large bowel, which absorbs excess water. The waste is then temporarily stored in the colon before it is eliminated from the anus.The two ways in which Crohns disease and ulcerative colitis disturb the digestion and absorption processes are:
- Crohns disease an inflamed ileum impairs absorption of vitamin B12 and bile salts. Inflammation along the length of the small intestine impairs absorption of all food nutrients. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
- Ulcerative colitis digestion and absorption are generally not affected. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
Other factors that may affect your nutritional status include:
Are Eggs Bad For Ulcerative Colitis
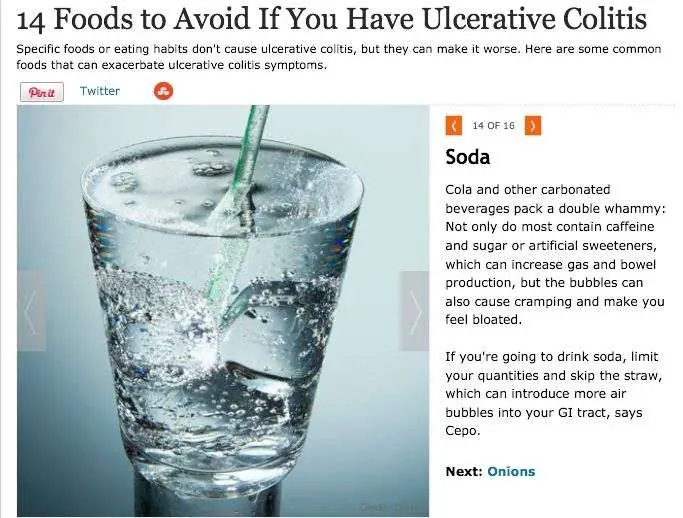
Eggs: These offer several essential nutrients, including omega-3 supplementation. They are typically easy to digest, which makes them good for an ulcerative colitis diet plan. Plenty of fluid: People with conditions such as ulcerative colitis may need to drink extra fluids, as diarrhea can lead to dehydration.
Read Also: What Can You Drink On Intermittent Fasting
The Miracle Of Juice Fasting For Crohns Disease Colitis Celiac And Ibs
- Posted onNovember 22, 2008
- inCeliac Disease, Colitis, Constipation, Crohn’s, IBS , Juicing
I enjoy a good meal and a glass of red wine as much as the next person so forgoing those two things has never been very high on my to-do list! But when you get sick with ulcerative colitis , you get so desperate, youll try anything.
I was born in Russia, and I knew that, for hundreds of years, supervised fasting has been used with great success as part of European medical treatments. The first time I personally tried fasting was in 1989. Twenty-one days of juice fasting together with medicinal enemas, nutritional supplements and herbs healed my supposedly incurable Pancolitis. My intestinal bleeding, chronic diarrhea, and joint pain vanished. I felt energetic and excited about being alive. Juice fasting saved my life and healed my soul.
I realized Hippocrates, the father of Western Medicine was right: fasting allows the body to heal itself.
Diet Recommendations For Crohn’s Disease Flare
- Follow a low residue diet to relieve abdominal pain and diarrhea.
- If you have strictures, it is especially important to avoid nuts, seeds, beans and kernels.
- Avoid foods that may increase stool output such as fresh fruits and vegetables, prunes and caffeinated beverages. Cold foods may help reduce diarrhea.
- If you have lactose intolerance, follow a lactose-free diet. Lactose intolerance causes gas, bloating, cramping and diarrhea 30 to 90 minutes after eating milk, ice cream or large amounts of dairy. A breath hydrogen test may confirm suspicions of lactose intolerance.
- If you have oily and foul-smelling stools, you may have fat malabsorption. Treat fat malabsorption by following a low-fat diet. Discuss these symptoms with your doctor or nutritionist.
- Smaller, more frequent meals are better tolerated and can maximize nutritional intake.
- If your appetite is decreased and solid foods not tolerated well, consider taking nutritional supplements .
You May Like: When Fasting How Many Calories
Intermittent Fasting: Putting The Pieces Together:
Intermittent fasting can seem daunting if youre used to eating from the time you wake to the time your head hits the pillow, but the body is perfectly capable of adjusting to, and thriving on, a more limited eating window. Youll likely find your digestive system loves it, and your mental clarity is at its peak great during your fasting window.
Consider giving it a shot if youve got digestive complaints, but just realize that its not the be-all-end-all solution. Youll probably need to improve your diet as well.
Inflammatory Bowel Disease Management
Inflammatory bowel disease is not caused, nor can it be cured, by what you eat. Doctors and dietitians agree, however, that food may play some role in the underlying inflammatory process that causes IBD symptoms.
Certain foods may aggravate symptoms, while others may calm them and promote healing. Therefore, paying attention to what you eat and how your body responds to different foods is an important component of a total treatment plan for IBD.
A diet plan can supplement but should never replace medical treatment for IBD. Always take your medications exactly as prescribed by your doctor.
Don’t Miss: How Should I Start Intermittent Fasting
Intermittent Fasting And Ibd: The Debate
While theres research showing that intermittent fasting can benefit people in the general population, studies in people with Crohns and ulcerative colitis are lacking.
Some studies have shown that intermittent fasting/time-restricted feeding may decrease inflammation and improve gut microbiome health, says Kelly Kennedy, a registered dietitian nutritionist with Everyday Health. But this research is still in its infancy.
Lack of research aside, many experts believe that people with Crohns disease shouldnt try IF, partly because they may already be deficient in certain nutrients or underweight.
Some studies have suggested that fasting in general though not intermittent fasting itself can lead to nutrient deficiencies, including protein. This is what an analysis published in October 2020 in the journal Nutrients found.
Limiting the amount of time you eat each day or even the number of days per week also limits the number of opportunities you have to get calories, vitamins, and minerals into your body, she says. This isnt a good idea for anyone who is underweight.
People with IBD can also be iron deficient, because theyve eliminated meat from their diet, she explains. About 1 in 3 people with IBD have anemia, a condition in which a person has less blood that can carry oxygen throughout the body, according to the Crohns & Colitis Foundation. The most common cause of anemia is low levels of iron.
Essential Oils For Ulcerative Colitis: Remedies And Precautions
Some effective essential oils for ulcerative colitis include peppermint oil, basil oil, patchouli oil, turmeric oil, among others.
Ulcerative Colitis is an inflammatory condition that affects your colon.
It causes inflammation and ulcer symptoms in your digestive tract.
Its a severe bowel disease. But its different from Crohns Disease or Irritable Bowel Disease. This inflammatory disease will make you weak and may create life-threatening conditions.
You may find it hard to pass stool as this disease may narrow the area of your intestine.
You may also have diarrhea, joint pain, and swelling in the colon, and scarring of the bile ducts and pancreas.
Theres no cure for this disease. Doctors may prescribe medications to handle the symptoms.
Besides, some essential oils for ulcerative colitis may help you manage the symptoms naturally.
Recommended Reading: What’s The Benefit Of Intermittent Fasting
Is Intermittent Fasting Good For Ulcerative Colitis
Intermittent fasting lowers gut inflammation to help improve inflammatory gut disorders such as Crohn’s disease, ulcerative colitis, and IBS. The idea of intermittent fasting can be overwhelming, but you’ll be pleasantly surprised at how easy it is especially compared to other types of eating plans.
Accordingly, can intermittent fasting cure autoimmune disease?
Intermittent fasting can reduce inflammation it’s been shown to do so for other autoimmune conditions such as multiple sclerosis . Intermittent fasting is also helpful for rheumatoid arthritis reducing both inflammation and pain .
Subsequently, question is, is keto bad for ulcerative colitis? The ketogenic diet is naturally low in FODMAPS . Thus, one of the reasons the ketogenic diet may reduce IBD symptoms is possibly due to the reduction of fermentable carbohydrate foods.
In this regard, how long does it take for ulcerative colitis to go into remission?
Remission might last for months or even years. You may go from a mild flare-up to a severe one and back again. Or, it may get more advanced and spread to other parts of your colon. Two main things affect how you feel: where you get inflammation and how severe it is.
Should you intermittent fast every day?
You May Like Also
How Is A Food Allergy Treated

One way to treat food allergies is by eliminating the offending foods from your diet. First, you need to figure out which foods cause you to react. You can do this by keeping a diary of everything you eat for a few weeks.
Look for foods that are hard for some people with IBD to tolerate, such as:
- milk and other dairy products
- eggs
- tree nuts such as walnuts, almonds, cashews, and pecans
- wheat
- fish and shellfish
- artificial sweeteners
Once youve identified a few possible trigger foods, cut them out of your diet. Then reintroduce the foods, one at a time, to see if your symptoms come back.
Its important to be under a doctor or dietitians supervision when you try an elimination diet. Cutting foods out of your diet could leave you lacking in important nutrients. Your dietitian might recommend you substitute other foods to get the nutrition you need or take a supplement.
Immunotherapy is another treatment for food allergies. Youll do this under the direction of an allergist. Your doctor will give you very small amounts of the food that triggers your reaction. Gradually, youll eat more and more of the food until your body begins to tolerate it.
You can also ask your doctor about probiotics, which are supplements containing healthy bacteria. A
Recommended Reading: Do You Need To Be Fasting For A1c
What Side Effects Of Ibd Can Cause Malnutrition
There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohn’s disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
Can Fasting Help Ulcerative Colitis
Researchers have found that fasting especially, intermittent fasting, can help Ulcerative Colitis and other inflammatory bowel diseases. Specifically, they studied three types of intermittent fasting: alternate day fasting , time-restricted fasting , and intermittent energy restriction .
The results of this study found that time-restricted fasting and intermittent energy restriction both suppressed inflammatory responses, helped in reversing colitis development, and improved gut barrier integrity. If you are thinking about fasting while you have Ulcerative Colitis, it may be beneficial. Before you start your fast , talk to your doctor so that they can assist you in making the best decision for you.
Read Also: What Foods To Eat On 16 8 Intermittent Fasting
The Influence Of A Fasting Mimicking Diet On Ulcerative Colitis
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government.Know the risks and potential benefits of clinical studies and talk to your health care provider before participating. Read our disclaimer for details. |
| First Posted : August 6, 2018Last Update Posted : May 4, 2021 |
- Study Details
| Inflammatory Bowel DiseaseDiet ModificationUlcerative Colitis | Other: Fasting Mimicking DietOther: Regular Diet | Not Applicable |
| Study Type : |
| The Influence of a Fasting Mimicking Diet on Ulcerative Colitis |
| Actual Study Start Date : |
| Three cycles of a 5-day reduced calorie diet | Other: Fasting Mimicking Diet5 day reduced calorie diet |
| Placebo Comparator: Regular Diet Control Arm | Other: Regular Diet |
Are Nutritional Needs Different For People With Ibd What Are The Specific Nutritional Needs For People With Crohn’s Disease And Ulcerative Colitis
Nutritional needs are specific to the individual and differ with disease state, body size and age. A nutritionist can help you estimate your individual needs. Calorie and protein needs are similar for Crohn’s disease and ulcerative colitis. In both diseases, needs increase during inflammation and immediately after to restore losses. The following are general statements about nutritional needs that may apply to you.
Read Also: Which Intermittent Fasting Schedule Is Best For Weight Loss
What Does Prednisone Do For Ulcerative Colitis
Prednisone is a steroid with anti-inflammatory effects. It is used to treat inflammation in ulcerative colitis and Crohns disease. However, steroids do not prevent symptoms from returning and have many side effects. Sometimes, it is necessary to use steroids to treat IBD, especially during flares.
What Is A Flare
When you have ulcerative colitis, your physician will try to find the right medications to control your symptoms. However, since there is no cure, the systemic disease is always there. When the symptoms arent present, you are in remission. If the symptoms return, especially if they are worse than before, it is a flare. This is why it is important to continue taking any medications your doctor prescribes, even if you feel better. If you stop taking your medication, then you can increase your chance of experiencing a flare and progression of the disease. Infections, stress, and taking antibiotics or NSAIDs can also make you more susceptible to a flare.
Read Also: Can I Have Coffee While Fasting
Should You Try Intermittent Fasting If You Have Crohns
Given the possible drawbacks of IF, experts are hesitant to recommend it for people with Crohns disease. This is especially true for people with severe Crohns who are unable to eat as much as they need to during a flare, explains Jeff D. Scott, MD, a gastroenterologist with Digestive Disease Specialists, Inc., and in private practice in Oklahoma.
Sabine Hazan, MD, a gastroenterologist and creator of ProgenaBiome a genetic sequencing research lab says that if people with Crohns want to try IF to see if it reduces their symptoms, they should alert their doctor first.
If a Crohns patient is trying intermittent fasting, I would certainly recommend working with a registered dietitian nutritionist who specializes in digestive conditions, says Kennedy. Its important that their weight and diet be tracked even more closely than usually recommended while on IF.
If fasting is causing you to lose out on vitamins and minerals or complicating your Crohns symptoms, you should stop, she says.
Even if you are modifying your diet to better control your symptoms, keep in mind that its not a substitute for medications and shouldnt be used to treat intestinal inflammation, Dr. Gaidos says.
Rather than fast, Gaidos tells people who have Crohns to eat a well-balanced, healthy diet that is low in processed foods and sugar. Diets lower in indigestible fiber may also be easier for your body to digest, says Dr. Scott.